Source: koya79/istockphoto.com
When you have an in vitro fertilization (IVF) cycle, the eggs and sperm are combined in the lab on the first day. There are two ways the eggs can be fertilized.
The first is by adding thousands of sperm around each egg and letting the process happen naturally; this is called conventional insemination and is done when the sperm count is good or there is previously proven fertility between the man and woman.
If there is any concern about the sperm’s ability to fertilize the eggs, the embryologist consults the physician who may make the decision to perform intracytoplasmic sperm injection (ICSI).
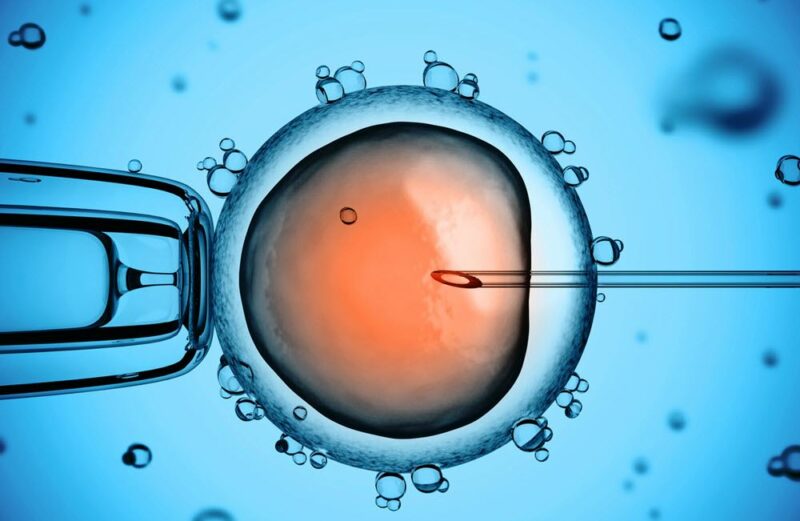
For ICSI, a single sperm that is the most morphologically normal looking is selected using a high-power microscope and injected into an egg. This is a very effective way to fertilize the eggs and ensures (to a degree) that the eggs will fertilize.
When is ICSI Recommended?
This procedure is generally used in cases where the male partner has:
- Low sperm count
- Low sperm motility (movement)
- Poor sperm morphology (shape)
- Surgically extracted sperm
- A vasectomy reversal
Some clinics may choose ICSI when there is unexplained infertility and are concerned whether the egg and sperm can bind properly during the acrosome reaction.
It is also possible to do ICSI on a portion of the eggs while also trying conventional insemination if there is some doubt about whether the eggs will fertilize naturally. In this situation, some eggs are inseminated with sperm; some are injected. If the sperm don’t fertilize the eggs naturally, the ICSI injected eggs are the “insurance.”
At some clinics, ICSI is done when frozen sperm is being used for an IVF cycle, if you are using a frozen sample, ask your doctor about the fertilization rates of frozen sperm versus fresh sperm at their clinic and whether ICSI is recommended.
Is ICSI Overused?
Trends in ICSI use show it is used in the majority of fresh IVF cycles in the USA. Some clinics exclusively use ICSI on all their patients to avoid the rare case where there is a fertilization failure after insemination. To some, this is an example of how ICSI is being overused and to others, it is seen as a safeguard against having no embryos for transfer.
What are the Risks of ICSI?
ICSI carries a small risk of damaging the eggs during the injection, although in good hands this happens in less than 5% of eggs. Because this is generally a technical issue, you can better understand the risks of the procedure by asking your clinic:
- What are your ICSI fertilization rates?
- What are your ICSI damage rates?
- Do I need to do ICSI in order to successfully fertilize my eggs?
What are the Costs Associated with ICSI?
Having ICSI usually adds on an extra cost to your IVF cycle, this can be in the region of $1,500 more. Ask your clinic about the cost of ICSI and any extra charges that may be added to your account such as blastocyst culture and assisted hatching.
Usually, you do not need to have ICSI if you are doing preimplantation genetic testing (PGT) on your embryos, especially if the embryologist is taking trophectoderm biopsies, although this can vary from clinic to clinic. Your clinic might recommend ICSI during a PGT cycle to make sure the chromosome results aren't contaminated.
Is ICSI Safe in the Long Term?
Many studies have followed the development of children conceived using ICSI to ensure the safety of this technique. Several major studies have shown that although fertility treatments themselves carry small risks, there is no difference in the occurrence of abnormalities between babies born from ICSI or standard IVF where the eggs were not injected.
What is not yet clear is whether genetic abnormalities are passed from father to son. For example, if the male partner has a chromosomal abnormality that causes low sperm count, this could be passed to the male children. Although the babies appear to be healthy and well, they may have inadvertently inherited a fertility problem themselves. This is yet to be seen on a large scale because of the small number of IVF-assisted babies that have had children of their own.