If you’re planning to undergo in vitro fertilization (IVF), you may have heard the term preimplantation genetic testing (PGT). It’s an option available to individuals or couples undergoing IVF, and it involves genetically screening the embryos before embryo transfer.
There are multiple types of PGT testing:
- Preimplantation Genetic Testing for Aneuplodies (PGT-A)
- Preimplantation Genetic Testing for Structural Arrangements (PGT-SR)
- Preimplantation Genetic Testing-Monogenic or Single Gene Disorders (PGT-M)
These tests can be done:
- To reduce miscarriage rates by transferring only genetically normal embryos
- To eradicate a genetic disorder from a family
- For the purpose of gender selection (although this is somewhat controversial)
- For patients who have a poor prognosis with IVF
If you’re curious about or are considering PGT, it can help understand how this testing is carried out and whether you are likely to benefit. Here we’ll take a look at PGT in-depth, starting with PGT-A.
What are chromosomes, and why do they matter for PGT-A?
To understand PGT-A genetic testing of embryos for aneuploidy, you must first grasp some basic cell biology. Each cell in the body has 46 chromosomes, except eggs and sperm, which each have 23. The egg and sperm combine to give the offspring a total of 46 chromosomes. We inherit half of our chromosomes from our biological father and the other half from our biological mother. These chromosomes act like instruction books and control the function of our cells.
If an egg or a sperm is missing a chromosome, then the embryo created from that egg or sperm will also be missing a chromosome and a whole set of instructions. If there is an extra chromosome in an egg or sperm, the embryo will be abnormal, having twice as many copies of those instructions then it should have. Down Syndrome is one example of a genetic disorder caused by an additional copy of a chromosome.

Most such embryos will not implant at all, some will cause an early miscarriage, and some can go to full term and be born. Almost all of the babies born with extra or missing chromosomes will have some kind of physical and/or mental disability.
Why undergo preimplantation genetic testing for aneuploidy (PGT-A)?
In most studies, preimplantation genetic testing has not been shown to improve pregnancy rates for the general population undergoing IVF. However, it has been shown to:
Genetic Counseling as Part of the PGT Process
If you are considering testing your embryos during an IVF cycle, you might be referred to a genetic counselor who will ask extensive questions about your family history. This counselor will also consider the age of the female partner and tell you your chances of having normal embryos during your IVF cycle. Many genetic laboratories will also review the fees and accuracy of the testing ordered by your doctor.
A genetic counselor and your doctor should discuss the pros and cons of testing your embryos as per your specific situation and whether it’s the right decision for you.
How Embryos Are Tested During PGT
It’s possible to test each embryo created by IVF and count the number of chromosomes.
This is done by:
- Taking cells from the embryo on day five, six, or seven, assuming it reaches the blastocyst stage of development. A blastocyst biopsy facilitates several cell tests, thereby reducing the risk of a false result.
- Freezing them and sending them to a genetics lab.
- The genetics lab will then run a test on those cells to determine if the embryo is chromosomally balanced.
If embryos are tested on day five or day six at the blastocyst stage, they usually have to be frozen because the results aren’t available in time for a fresh transfer. A few clinics offer overnight testing, and this option may become more available with time and better technology.
Some clinics offer to test the “spare” embryos from an IVF cycle. In this case, you get a fresh transfer of untested embryos, and any extra embryos of suitable quality will be biopsied before being frozen.
PGT and Embryo Growth
The removal of cells from the embryo at these early stages does not affect the embryo or fetal development. The embryo can usually compensate for the damage within a few cell divisions. In good hands, the biopsy of an embryo has little effect on its growth, although it may slow down slightly.
That said, the biopsy itself is invasive, and there is a chance that a normal embryo that would have otherwise implanted could be damaged beyond repair. This is a major risk in PGT: it can compromise the viability of the embryo tested. Note that this will not lead to abnormalities in a baby. In this case, the embryo has been damaged so that it is no longer able to implant.
If no embryos develop to the blastocyst stage of development, no testing can or will be performed.
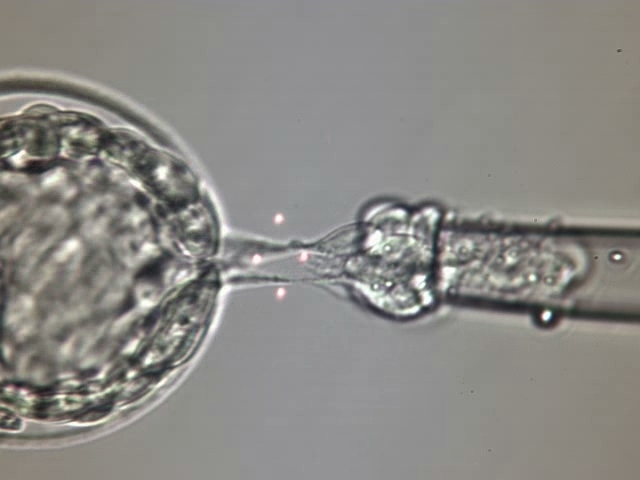
Embryo Biopsy for PGT
Cost Is a Major Consideration for PGT
Another thing to consider with PGT is that it incurs additional fees on top of those charged for your regular IVF cycle. In general, the cost of PGT includes three fees:
- Biopsy fee charged by your IVF clinic
- Shipping fees for frozen biopsy cells charged by your IVF clinic
- Testing fees charged by the genetic testing lab
All these charges are refundable if there are no embryos to biopsy. The total cost for embryo testing is in the region of $5,000, not including the cost of frozen embryo transfer cycles that will be incurred to transfer the tested and balanced embryos. This can also be several thousand dollars.
Remember that so far, data have shown that women over 38 are most likely to benefit from embryo testing, whereas younger women may have better success without it.
The Limitations of PGT Genetic Testing
PGT does have some limitations. PGT testing is another screening method. It gives the embryologist and doctor another piece of information on which embryo has the highest implantation potential. Much can go wrong, including:
- No embryos form blastocysts for biopsy
- The blastocyst could not survive the biopsy
- No blastocysts come back transferrable
- The blastocyst could not survive the freezing and thawing
It is important to remember this procedure is not reparative and can only identify an imbalance but not fix it.
Another important consideration is the rationale behind the test is the presumption that each cell in the embryo is genetically identical. In other words, if you test one cell from the embryo, you know what all the other cells are. However, there have been reports of embryos exhibiting mosaicism, where not all the cells in the embryo are identical. This leaves open the possibility of misdiagnosis and the discarding of normal embryos or the transfer of abnormal embryos.
Because most genetically abnormal embryos stop growing before the blastocyst stage or fail to implant, most women do not have increased pregnancy rates following PGT. The outcome of the IVF cycle is likely to be the same with or without the testing. The main difference is that by doing PGT, you have the information before an embryo transfer rather than after. PGT can help women struggling to decide whether to continue to use their own eggs after several failed IVF cycles, and there is a real possibility there could be no normal embryos for transfer.
The Potential Pros of PGT
- It allows lab personnel to identify if there are any balanced embryos for transfer for women of advanced maternal age or with repeated implantation failure or miscarriage. This will lead to a faster time to pregnancy for women in this group because it avoids monthly cycling and pregnancy tests.
- It saves time and money by avoiding the transfer of embryos that are genetically abnormal in frozen embryo cycles.
- It reduces miscarriage rates.
- It provides information to help you make decisions about future treatments
- It can help avoid the need for invasive testing once pregnant
- It can provide peace of mind
- It can reduce the number of embryos transferred and better utilization of elective single embryo transfers.
- You will likely be provided the sex of the embryos tested
The Potential Cons of PGT
- There is usually no improvement in pregnancy rates for younger women with a good chance of success. In young, healthy women, testing may decrease the chances of success because the embryos have to go through an invasive biopsy and freezing process, both of which can damage them to some degree.
- Normal embryos could be damaged during the biopsy. The biopsy itself is invasive, and there is a chance that a normal embryo that would have otherwise implanted could be damaged beyond repair.
- Normal embryos could be damaged during freezing. At this time, all PGT embryos str usually frozen until the results from the genetic testing have been processed. This additional step of freezing and thawing the embryo can further compromise its potential for pregnancy.
- Results may not be 100% reliable.
- The cost could be prohibitive for some individuals or couples.
- You must pay for a subsequent frozen embryo transfer cycle if you choose to freeze all your embryos.
- Theoretically, it does not eliminate the need for prenatal testing.
- The need to discard viable but genetically unbalanced embryos.
How are embryos chosen for transfer following PGT?
If you decide to undergo PGT, the embryos chosen for transfer have to be:
- Genetically normal
- The sex of the embryo is potentially a consideration
- Have a normal pattern of growth
- Survive the freeze-thaw process
There is no point in transferring an embryo that has stopped growing or did not survive the thaw, even if the genetic analysis comes back normal. In other words, there is always a chance of not having an embryo transfer regardless of the PGT results.
PGT and Maternal Age
Because PGT is not without risk to the embryo, it is important to consider who is most likely to benefit from the procedure. Data collected so far have shown that the risks outweigh the benefits for younger women (the pregnancy rates are lower with testing). But for women aged 38+, the benefits outweigh the risks, and we see improved pregnancy rates for this group.
Your Options for Genetic Testing of Your Embryos
No Testing
In this case, both the embryo/s transferred in the fresh cycle and subsequent frozen embryo replacement cycles have unknown chromosomes. You then have the option to do genetic testing on the baby after a pregnancy is established while it’s growing in the womb. This is the best option for young women who have a good chance of success.
Test Spare Embryos Only
In this case, the embryo/s transferred in the fresh cycle have unknown chromosomes. Any subsequent frozen embryos transferred are tested. This saves time and money storing or transferring embryos that are chromosomally abnormal and should improve the pregnancy rate for the frozen embryos transferred. This option is best if you want good information about your spare embryos, have a good chance of success without genetic testing with your fresh embryos, are interested in reducing the chance of a pregnancy/child with an abnormality in chromosome number, or are interested in knowing the sex in future cycles.
Test All Embryos
Testing of all embryos is generally recommended if you want as much information as possible before the transfer, are interested in reducing the chance of a pregnancy/child with an abnormality in chromosome number, are of advanced reproductive age, have had two or more miscarriages, have gone through multiple failed IVF cycles, have a previous pregnancy or child with an abnormality in chromosome number or must freeze all of your embryos anyhow.
Bank Embryos
Some IVF cycles produce only one or two embryos of suitable quality for testing. In this case, you can choose to freeze the embryos and undergo another IVF cycle in the hope of having additional embryos to test. This is called embryo banking. It’s a cost-effective way to test embryos from several IVF cycles as you pay the testing fee only once. The embryos can be frozen before or after a biopsy, depending on your clinic’s procedures.
PGT and a ‘No Diagnosis’ or ‘Mosaic’ Result
Sometimes embryos that undergo PGT have a “no diagnosis” result. This means that the test failed for a particular embryo. Some couples choose to transfer these embryos anyway, despite not obtaining any information about that particular embryo.
Sometimes embryos that undergo PGT have a “mosaic” result. This means there was a mixture of normal and abnormal cells. Most clinics do not allow the transfer of mosaic embryos at this time.
Preimplantation Genetic Testing-Structural Rearrangements (PGT-SR)
PGT-SR can also be used to detect translocations in the embryos, which are changes in the structure of the chromosomes. Changes are quite rare but do account for some cases of recurrent miscarriage or implantation failure. It’s estimated that around 1 in 625 people carry a translocation. PGT-A can usually be combined with this type of testing since one biopsy sample can be used for both types of testing.
If you have suffered multiple miscarriages or multiple failed IVF cycles, it might be a good idea to talk to your doctor about checking the structure of the chromosomes for translocations in the female and the male partners.
Preimplantation Genetic Testing-Monogenic or Single Gene Disorders (PGT-M)
At any stage, you may be offered testing for inherited genetic disorders caused by mutations in a single gene. These can be diseases that lie dormant in DNA and could be passed onto a child if both partners carry the same recessive genes.
As many illnesses are attributed to a genetic source, more screening options arise (BRCAA for breast cancer, etc.). Embryos can also be screened to identify human leukocyte antigen (PGT-HLA) matching using this type of testing. This makes it possible to identify embryos that are HLA compatible with a child in need of a bone marrow transplant.
PGT-A vs. PGT-M
PGT-A counts the overall number of chromosomes, but PGT-M identifies a specific gene in a preimplantation embryo.
Genetic disorders are often caused when a gene mutates or the instructions have become misspelled on the part of the DNA. This causes the cell to malfunction and not produce the correct proteins needed to do a specific task in the body. Genetic diseases of this type are called single-gene disorders.
A person who carries this type of genetic disorder can undergo a cycle of IVF. This presents an opportunity to create offspring that may not be affected by this disorder. The accuracy of the results is close to 100%.
Although PGT carries some risk of damaging the embryo during a biopsy, for some, this risk is offset by the peace of mind in knowing a child will not exhibit symptoms of a potentially debilitating or even lethal disease.
PGT can detect the following diseases and many more:
- Cystic fibrosis
- Sickle cell anemia
- Tay-Sachs disease
- Myotonic dystrophy
- Muscular dystrophy
- Fragile X syndrome
- Spinal muscular atrophy
- Huntington’s disease
- Hemophilia
In PGT testing, cells are removed from each embryo during early development, and the DNA is multiplied many times. A specially developed probe is then used in the specific region of DNA (or gene) that carries the disease mutation. The lab identifies the results of which embryo is transferable. It is often combined with PGT-A since one biopsy sample can be used for both types of testing.
Choosing the Sex of Your Baby with PGT
Preimplantation genetic testing can be used to detect the sex of the embryos when a baby of a certain sex is desired. Even though this is a controversial use of reproductive technology, most clinics offer this as a service. Some clinics have restrictions on which families they allow to choose the gender. They may require a couple to have children already and want a child of the opposite sex. This is called family balancing.
During an IVF cycle, the embryos are biopsied and analyzed the same way as in PGT-A testing. The other chromosomes can also be tested at the same time to ensure the genetic normalcy of the embryo, as well as sex.
When the genetic testing results arrive, you are told the results of the genetic analysis and the quality of the embryos. It’s possible that there may not be good-quality embryos of the desired sex. In this case, you would have to decide whether to transfer the alternate sex or lower-quality embryos.
Should you choose PGT?
This is a very personal question that each individual or couple must weigh based on information from their fertility treatment team. PGT has been shown to have benefits for women of advanced maternal age. It can also reduce miscarriage rates, and multifetal pregnancies and provide peace of mind.
The downside of doing PGT is that there is a potential of disrupting the embryo growth by doing the biopsy or freeze. The procedure is also very costly and may not provide completely comprehensive results.